What Do Occupational Therapists Address in Schools?
Occupational therapy in educational settings is much broader than handwriting practice. School-based OTs evaluate and support any skill that affects a student’s ability to access, participate in, and benefit from their education. Under IDEA (2004), OT is a related service — meaning it must be provided when a student’s disability affects their educational performance and OT support will help them benefit from special education.
In practice, this means OTs work on the physical, sensory, cognitive, and social-emotional skills that underpin daily school tasks: writing a paragraph, navigating a cafeteria, managing transitions, regulating emotions, and participating in group activities. For students with IEPs, OT goals and recommendations are legally binding components of the plan that must be implemented by the entire team — not just the therapist.
What Are the 13 Core OT Areas of Concern in Schools?
The occupational therapy recommendations in this resource cover the 13 most frequently documented areas of concern in school-based OT evaluations. Each area includes a precise clinical description, a realistic classroom example, and evidence-based recommendations with peer-reviewed references.
Precision hand movements — gripping, pinching, bilateral coordination. Affects writing, cutting, and self-care tools.
Large-muscle coordination — running, balance, posture. Affects PE, navigation, and desk sitting endurance.
Legibility, sizing, spacing, and writing speed. May require OT evaluation for formal dysgraphia identification.
Registration and modulation of tactile, vestibular, auditory, and proprioceptive input. Basis of the Sensory Diet® model.
Dressing, feeding, hygiene, and grooming. Targeted through backward chaining and adaptive equipment.
Form constancy, figure-ground, spatial relations, and visual-motor integration. Evaluated using TVPS-4 or Beery-VMI.
Proprioception and body scheme. Heavy work activities and movement breaks are first-line strategies.
Planning, initiation, cognitive flexibility, working memory. Addressed via CO-OP Approach and visual scaffolds.
Arousal regulation — both hypo and hyperarousal states. Alert Program® and sensory environment optimization.
Imaginative, exploratory, and cooperative play. DIR/Floortime® and JASPER are evidence-supported models.
Turn-taking, joint attention, perspective-taking. Social Thinking® and Social Stories™ are the leading frameworks.
Modulating and expressing emotions. Zones of Regulation® with sensory-based co-regulation strategies.
Flexibility with routine changes and novel environments. Linked to interoception, PDA profiles, and cognitive rigidity.
Preview — OT Issues & Recommendations Chart 2026
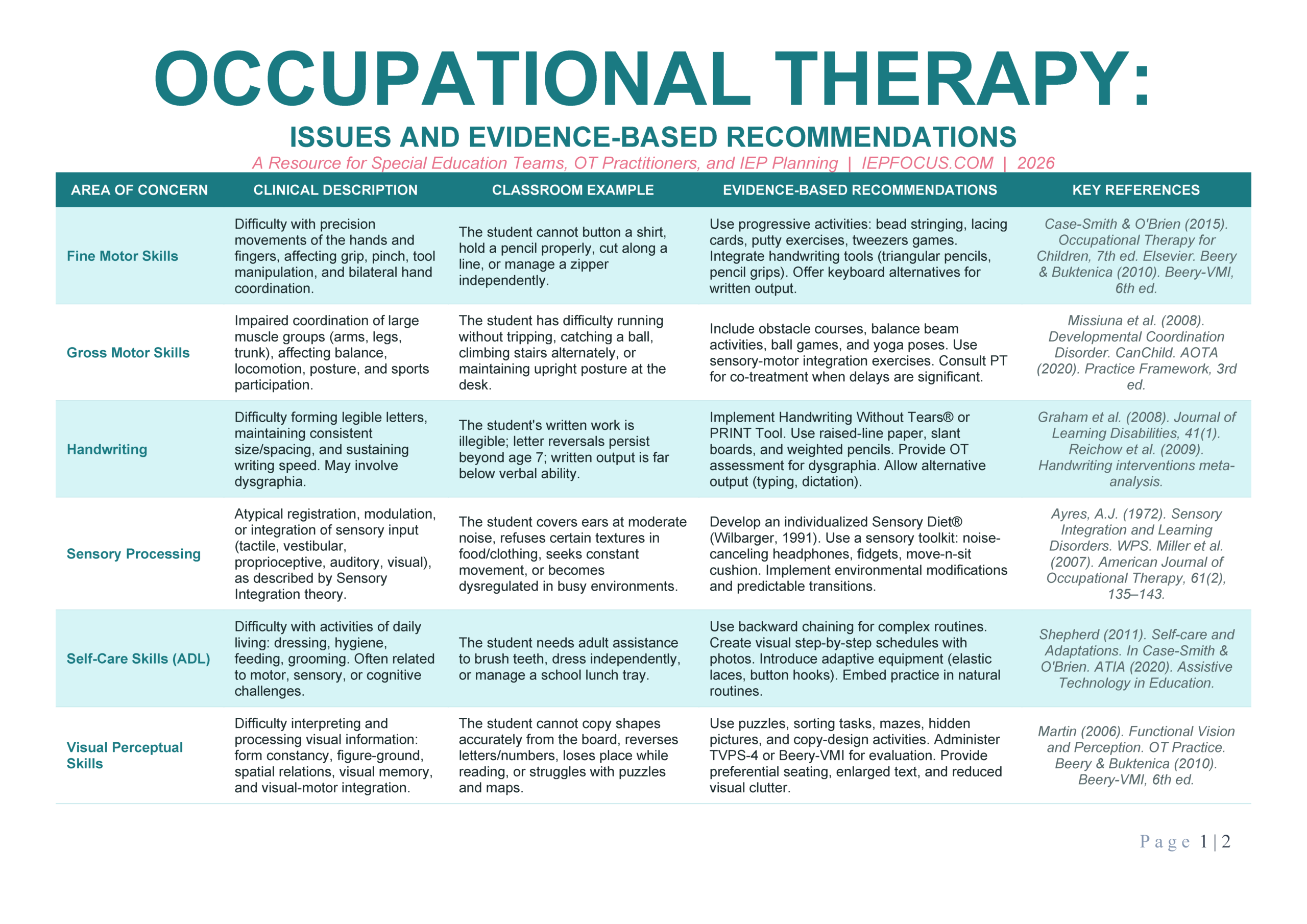

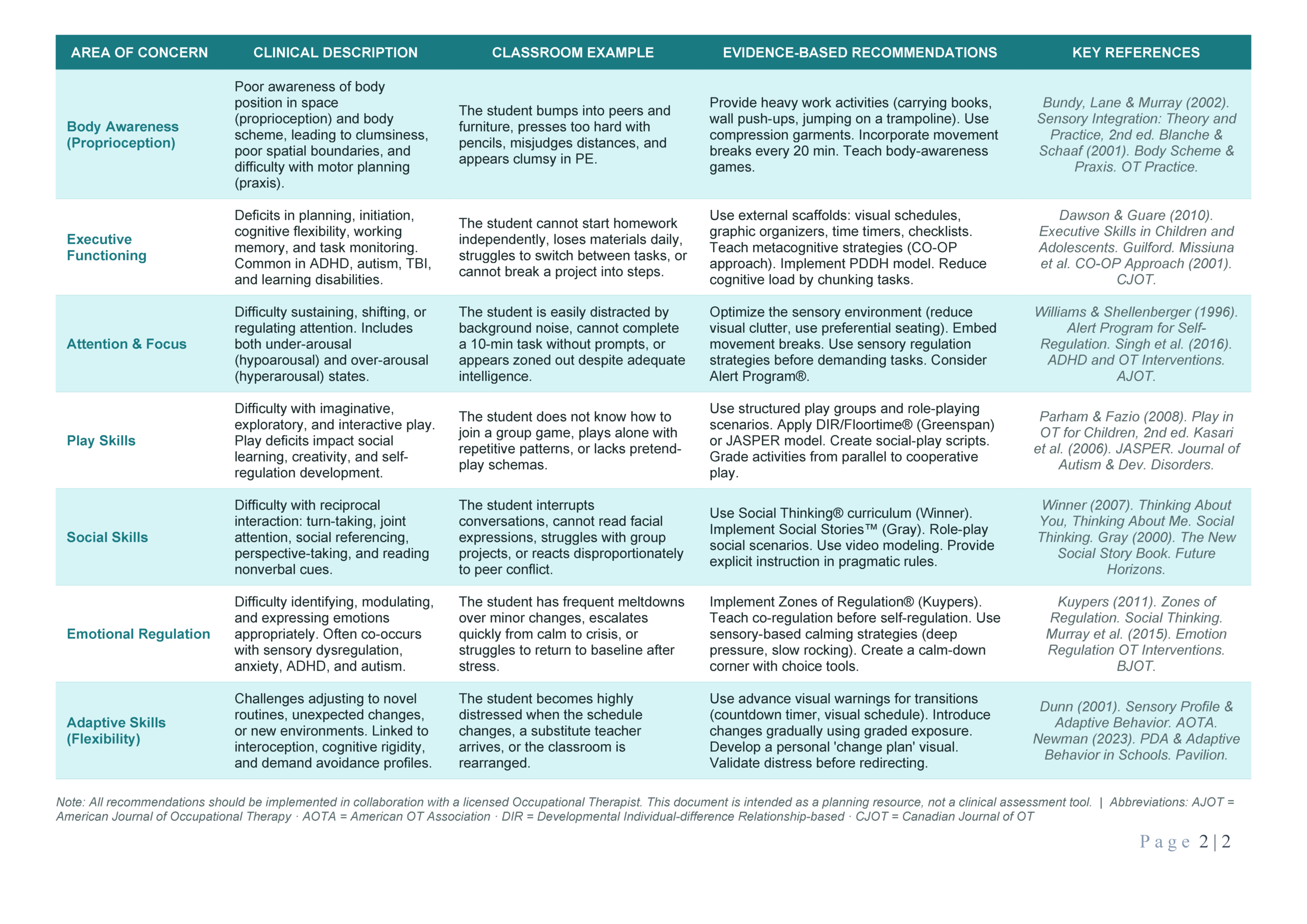
Click the images to enlarge · Full interactive version below
Browse the full chart below, then save or print it directly from the viewer.
How Should Teachers Use Occupational Therapy Recommendations in the Classroom?
IN CLASS OT recommendations only work when they are consistently implemented — not just during pull-out sessions. Research consistently shows that embedded, naturalistic implementation produces greater skill generalization than isolated therapy alone (Case-Smith & O’Brien, 2015). Here is how to translate the chart into daily classroom practice:
Set Up the Environment Before the Student Arrives
Many OT recommendations are environmental, not behavioral. Before the school day, scan your room through an OT lens: Is the seating height correct for the student’s feet to rest flat? Is there visual clutter on the walls that competes for attention? Is there a quiet corner available for sensory regulation? Small environmental adjustments reduce the frequency of dysregulation without requiring any intervention in the moment.
Embed Movement Into Your Schedule
For students with body awareness, attention, or sensory processing challenges, movement is not a reward — it is a regulatory tool. Research supports movement breaks every 20–30 minutes for students with ADHD and sensory needs (Singh et al., 2016). These do not need to be long: 3-minute brain breaks, errand tasks (delivering attendance to the office), or standing desk options are all effective and minimally disruptive.
Use Visual Supports for All Executive Functioning Goals
If a student’s IEP includes OT goals around executive functioning — initiating tasks, organizing materials, completing multi-step work — visual schedules and checklists are the most accessible classroom implementation tool. Post the daily schedule prominently, use a visual checklist for homework packing, and provide graphic organizers for any written assignment with more than two steps.
| OT Area | Quick Classroom Strategy | Takes Less Than… |
|---|---|---|
| Sensory Processing | Provide a seated fidget tool or wobble cushion | 2 minutes to set up |
| Fine Motor | Offer pencil grips and triangular pencils | 0 minutes — just stock them |
| Attention | Seat the student near the front, away from windows | 1 minute to rearrange |
| Body Awareness | Add a 3-min movement break after every 25 min of work | 3 minutes per break |
| Executive Functioning | Post a visual “End of Day” checklist on the student’s desk | 5 minutes to make |
| Emotional Regulation | Set up a calm-down corner with 3 tool choices | 15 minutes to assemble |
What Can Families Do to Support OT Recommendations at Home?
AT HOME When families understand the “why” behind OT recommendations, they become the most powerful implementers on the team. The challenge is that OT reports are often written for clinicians, not parents. This chart was specifically designed with plain-language descriptions and real-life examples so families can immediately see themselves in the content.
Routines Are the Most Powerful OT Tool at Home
For students with adaptive skills challenges, sensory processing differences, or executive functioning needs, a predictable home routine is not optional — it is therapeutic. Consistent morning and evening sequences reduce the cognitive load of transitions and give the nervous system a sense of safety. Visual schedules work just as well at home as at school: a simple printed sequence of “Wake up → Brush teeth → Get dressed → Eat breakfast” posted in the bedroom eliminates most morning battles for many families.
Embedded Practice Beats Drilling
Cooking, setting the table, sorting laundry, and playing with building toys are all occupational therapy. Fine motor, self-care, and executive functioning skills develop fastest when practiced in meaningful, motivating contexts — not worksheets. Ask your child’s OT for a home activity menu tied to their current IEP goals, and embed those activities into daily routines your family already does.
Advocacy Tip: Ask for a Home Program at Every IEP Meeting
Under IDEA, IEP teams are required to discuss how parents can be involved in supporting their child’s goals. Families can — and should — request a written home program from the OT at every annual review. This program should list 3–5 activities, explain how to do them, and describe what “progress” looks like so parents can observe and report back to the team.
How Do Occupational Therapy Recommendations Connect to IEP Goals?
LIFE OT recommendations in an evaluation report are not automatically IEP goals. They become goals only when the IEP team — including the OT, the special educator, the family, and (where appropriate) the student — agrees that a specific skill is an educational priority. Understanding this distinction is critical for advocates and families.
The occupational therapy areas in this chart map directly onto the most common IEP goal domains: fine motor and handwriting goals appear under Present Levels of Academic Achievement; sensory and regulation goals appear under Social-Emotional or Behavioral needs; executive functioning goals may span multiple areas. If your student has an OT evaluation on file, use this chart to cross-reference the evaluation findings with the goals currently written in the IEP — gaps between identified needs and written goals are one of the most common IEP compliance issues teams encounter.
13 areas · Clinical descriptions · Evidence-based strategies · Peer-reviewed references · 2026 Edition.
Frequently Asked Questions About OT Recommendations for Students
School-based OT services are provided under IDEA and must be educationally necessary — meaning they support the student’s access to and benefit from education. Private OT addresses the child’s overall functional development in daily life and is not limited to educational goals. Many students receive both; the goals should be coordinated but are legally and clinically distinct.
Yes. Under IDEA, parents have the right to request an initial evaluation in any area of suspected disability, including OT-related areas. The request must be made in writing to the school district. The district must respond within 60 days (varies by state) with either an evaluation plan or a written refusal explaining why they believe an evaluation is not warranted.
Common standardized assessments include the Beery-VMI (visual-motor integration), TVPS-4 (visual perception), Sensory Profile 2 (sensory processing), Bruininks-Oseretsky Test (motor proficiency), and the Peabody Developmental Motor Scales. OTs also use clinical observation, teacher and parent questionnaires, and functional task analysis.
OT goals are reviewed at every annual IEP meeting, but best practice calls for progress monitoring at least every 6–8 weeks. If a student is not making expected progress on an OT goal, the team should meet to discuss whether the strategies need to be modified — this does not require waiting for the annual review.
Yes. The 13 areas in this chart are the areas most commonly flagged in OT evaluations for autistic students, students with ADHD, and those with AuDHD profiles. Sensory processing, emotional regulation, adaptive skills, and executive functioning are particularly relevant for these populations. All recommendations follow a neuroaffirmative framework — no compliance-based or punitive strategies are included.
