Table of Contents
- Why Traditional Discipline Fails During a Crisis
- Understanding the Escalation Cycle
- The BERMED De-Escalation Framework: 6 Steps
- IN CLASS: Classroom-Based Strategies
- AT HOME: Strategies for Parents
- LIFE: Regulation Across Adolescence and Beyond
- What To Do — What To Absolutely Avoid
- Connecting De-Escalation to the IEP
- Frequently Asked Questions
- 5 Actions You Can Take Tomorrow
Most teachers intervene too late — and too loudly. By the time a student is yelling, throwing materials, or has shut down completely, the window for de-escalation has already passed. Research published in the Journal of Emotional and Behavioral Disorders found that 68% of escalated classroom incidents could have been prevented if staff had identified and responded to early warning signs within the first 90 seconds. The problem isn’t that teachers lack compassion — it’s that most received zero training in the specific, sequenced techniques that actually interrupt a behavioral storm. This guide gives you that sequence, step by step.

Why Traditional Discipline Fails During a Crisis
The most common mistake educators make during an escalating moment is continuing to talk. Issuing instructions, explaining consequences, or restating rules while a student is dysregulated floods a nervous system that can no longer process language. According to CHADD’s educator resource center, students with ADHD, autism, or trauma histories are especially prone to what neurologists call an “amygdala hijack” — a state in which rational thought is physiologically unavailable.
The result: the teacher escalates with the student. Both parties become dysregulated. The situation ends in punishment that damages trust, teaches nothing, and guarantees the next incident will happen sooner.
Understanding the Escalation Cycle
The escalation cycle, adapted from PBIS frameworks and Walker’s Acting-Out Behavior Model, gives teachers a map. Each phase requires a different response.
← Scroll to see full table
| Phase | What You See | What NOT to Do | Effective Response |
|---|---|---|---|
| Calm | Engaged, cooperative, on-task | Take for granted | Build relationship, teach skills proactively |
| Trigger | Slight tension, brief off-task behavior | Issue warnings or threats | Proximity, non-verbal check-in, offer choice |
| Agitation | Fidgeting, avoiding work, tense body, mumblings | Continue demands, call out publicly | Reduce demands, offer sensory break, quiet check-in |
| Acceleration | Arguing, voice rising, defiant responses | Escalate verbally, add consequences | Non-engagement, neutral tone, space and time |
| Peak | Full meltdown, physical behavior, shutdown | Reason, punish, restrain unnecessarily | Safety first, minimum verbal, environment management |
| De-escalation | Intensity decreasing, crying, withdrawal | Process immediately, demand apology | Quiet presence, offer water, no demands |
| Recovery | Calmer but fragile, may feel shame | Revisit incident right away with lecture | Reconnect first, debrief later, problem-solve collaboratively |

The BERMED De-Escalation Framework: 6 Steps
The B·E·R·M·E·D Protocol
Six sequential steps. Use them in order during an escalating moment. Each step builds on the one before it.
B — Breathe: Regulate Yourself First
You cannot co-regulate a dysregulated student if your own nervous system is activated. Before any intervention, take one slow breath. Soften your face. Lower your shoulders. Your body language is the first message the student receives.
Classroom scenario: Marcus, 7th grade with AuDHD, has just swept his materials off the desk. Your first impulse is to raise your voice. Instead: pause, breathe, drop your shoulders. Your regulated presence is already an intervention.
E — Environment: Reduce the Sensory and Social Load
Clear the physical space. Ask other students to quietly work independently or step into the hallway for a brief activity. Reduce noise, visual clutter, proximity of peers. A student cannot calm down while being watched by 28 classmates.
This step often requires a pre-established classroom routine — students know what to do when a peer needs space. Practice this routine proactively, not in the moment.
R — Reduce: Lower Demands to Zero
Remove all academic and behavioral demands immediately. Do not issue instructions. Do not remind the student of the rules. Do not reference consequences. The student’s only job right now is to exist. Your only job is to be present without pressure.
What this sounds like: Silence. Or: “No expectations right now. We’re just here.” Nothing more.
M — Match: Use Their Pace, Not Yours
Match the student’s energy level — then gradually lower it. If they’re speaking fast and loud, don’t respond with whispered calm immediately; it creates cognitive dissonance. Begin at a slightly lower volume and pace than theirs, then slowly reduce further over the next 60–90 seconds. This is called pacing and leading, and it works with the nervous system’s natural mirroring response.
E — Empathize: Name the Emotion Without Judgment
Once the student’s intensity has begun to drop (usually visible in the shoulders and face), offer a simple, non-interrogating empathy statement. Not a question. Not a demand. A reflection.
Examples: “That felt really unfair.” / “Something got really big right now.” / “I see you. We don’t have to figure it out yet.”
Avoid: “I understand how you feel” (often perceived as dismissive), “Why did you do that?” (demands linguistic processing before the brain is ready), or “You need to calm down” (creates shame).
D — Debrief: Problem-Solve When Calm Is Restored
The debrief happens later — ideally the next day, or at a scheduled quiet check-in. Not immediately after the incident. The goal is collaborative problem-solving: What triggered it? What helped? What can we plan for next time?
This step is where learning actually happens. It also models accountability without shame — the student participates in building their own support plan.

IN CLASS: Behavior De-Escalation Strategies for Teachers
Proactive Classroom Architecture
The most powerful de-escalation happens before a behavior begins. PBIS.org research on tiered supports consistently shows that clear routines, predictable transitions, and regulated sensory environments reduce behavioral incidents by 30–50% in SPED settings.
Set up your classroom with de-escalation in mind: a designated calm corner or regulation station (not a punishment corner), flexible seating options, reduced visual clutter near exits, and a simple signal system students can use to communicate overwhelm without speaking (a colored card, a specific object on their desk, a hand gesture).
Co-Regulation Routines Built Into the Day
Teach regulation strategies explicitly during calm moments. Morning meetings with a brief breathwork activity. Transition protocols that include 30 seconds of quiet before switching tasks. A “regulation menu” posted in the room: movement break, fidget tool, cold water, quiet corner, drawing, deep breathing.
Students with autism, ADHD, or anxiety cannot reliably access coping skills they’ve never practiced. Co-regulation routines turn strategies into habits before they’re needed under stress.
The Quiet Intervention Technique
When you notice early agitation signs (tapping, avoidance, increased movement), move toward the student calmly. Position yourself beside them, not in front. Speak at a low volume directly to them — not to the room. Offer a brief private choice: “Do you want to take a quick walk or use the calm corner for 3 minutes?” Then move away. Give them time to decide without you watching.
AT HOME: What Parents Can Do During an Escalating Moment
The Hardest Part: Not Escalating With Your Child
When a child is screaming, throwing objects, or completely shut down, a parent’s nervous system activates too. This is biological — mirror neurons, threat response, adrenaline. The most important thing a parent can do in those first seconds is pause. One breath. Shoulders down. Face soft.
Research from the Child Mind Institute on self-regulation in children confirms that the single most effective factor in reducing a child’s escalation at home is a calm caregiver presence. Not the right words. Not the right consequence. Calm.
A Simple Home Protocol
When an escalation begins at home, use the same BERMED sequence adapted for family context: Breathe (your breath, not a demand that they breathe). Environment (reduce noise, screens, siblings in the space). Reduce (drop all demands — homework, dishes, apologies — for now). Match and lower their energy. Empathize without interrogating. Debrief the next morning over breakfast, not at bedtime.
What to Tell Siblings
Prepare neurotypical siblings with age-appropriate language: “When [sibling] is having a hard moment, we give them space. That’s how we help. It’s not dangerous — it’s just their brain needing time.” This prevents peer escalation and teaches empathy as a household norm.
Communication With the School
Ask for a copy of any Behavior Intervention Plan (BIP) your child has. The same de-escalation strategies used at school should be mirrored at home — consistency across environments is the most powerful predictor of long-term regulation improvement. If no BIP exists and your child escalates regularly, request a Functional Behavior Assessment (FBA) in writing.
LIFE: Emotional Regulation for Neurodivergent Adolescents and Adults
Understanding Your Own Escalation Cycle
For neurodivergent adolescents and adults, self-awareness of the escalation cycle is a foundational skill. What are your personal early warning signs? Racing thoughts, sudden heat in the chest, jaw clenching, urge to flee? Knowing your body’s alarm signals gives you a 30–60 second window to intervene on your own behalf.
Keep a simple personal escalation log for two weeks: what triggered the moment, which phase you reached, what helped, what made it worse. Patterns emerge quickly. Self-knowledge replaces reactive shame with proactive strategy.
Building a Personal Regulation Toolkit
A toolkit that works for one neurotype may fail for another. Autistic adults may find deep pressure, rhythmic movement, or controlled sensory input most effective. Adults with ADHD may need physical activity, cold water, or a change of environment. Those with anxiety may respond best to structured breathing or progressive muscle relaxation.
The key is testing strategies during calm periods — not expecting to discover what works in the middle of a crisis. Practice them until they become automatic.
Workplace and Social De-Escalation
In professional settings, the same principles apply. Recognizing early activation signs, having an exit plan (“I need 5 minutes”), communicating needs before a crisis point, and choosing when and how to debrief afterward are all skills that can be developed and disclosed as workplace accommodations when needed.
ADDitude Magazine’s clinical coverage of emotional dysregulation in adults emphasizes that naming this as a neurological pattern — not a personality flaw — dramatically changes self-compassion and strategy adoption.
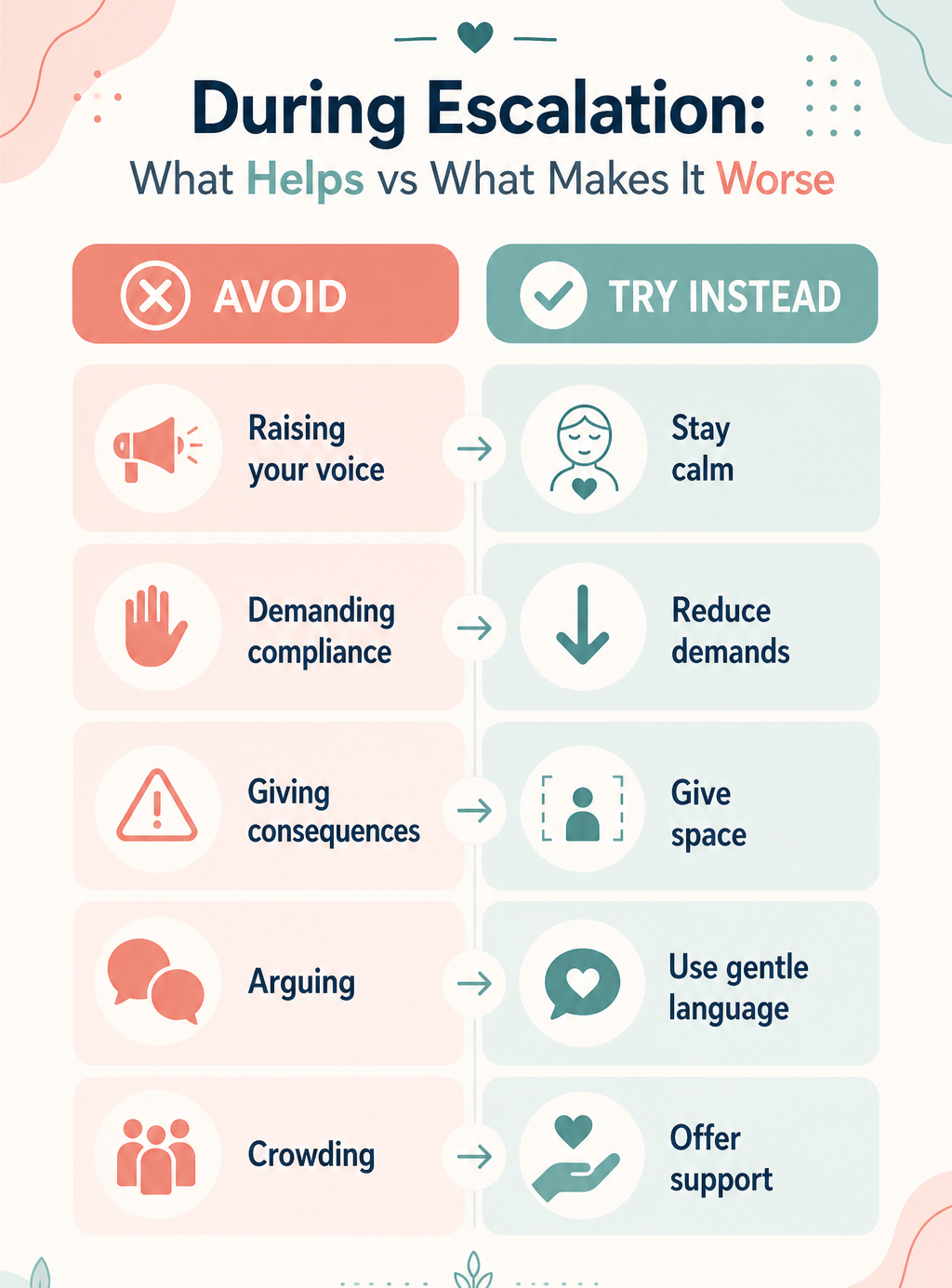
What To Do — What To Absolutely Avoid
✔ Do This
- Regulate yourself first
- Reduce demands immediately
- Lower your voice and slow your speech
- Move peers out of the space if possible
- Use non-verbal signals over verbal commands
- Offer one simple choice
- Stay nearby without crowding
- Name the emotion, not the behavior
- Wait for calm before processing
- Use the debrief to build the plan together
✗ Never Do This
- Talk more when the student is escalating
- Issue consequences during the peak
- Demand eye contact
- Call out the student in front of peers
- Tell them to “calm down” or “relax”
- Ask “why” during the crisis
- Take behavior personally and mirror the intensity
- Demand an apology at the moment of recovery
- Use physical restraint except for immediate safety
- Process immediately after the peak (wait at least 20 min)
Connecting De-Escalation to the IEP
What to Include in the BIP
A strong Behavior Intervention Plan includes the student’s specific escalation cycle warning signs, identified triggers, the de-escalation protocol to use at each phase, the environment modifications required, the staff member(s) trained in the plan, and the debrief process. It is not a list of consequences — it is a regulation support document.
IEP Goal Language for De-Escalation
When a student’s behavioral regulation is a goal area, write it in positive, measurable terms focused on skill-building rather than behavioral suppression. Examples:
← Scroll to see full table
| Weak Goal (Avoid) | SMART Goal (Use This) |
|---|---|
| “Student will reduce outbursts in class.” | “When experiencing escalating emotions, [Student] will use a self-selected regulation strategy (movement, tool, quiet space) independently in 4 out of 5 observed opportunities by May 2027.” |
| “Student will follow classroom rules.” | “[Student] will signal emotional dysregulation to a trusted adult using the agreed classroom signal system before reaching peak escalation, in 3 out of 4 trials, across 8 consecutive weeks.” |
| “Student will calm down within 5 minutes.” | “[Student] will identify 2 personal early warning signs and initiate a coping strategy from their regulation menu in 4 out of 5 opportunities, measured across 6 weeks of data collection.” |
The FBA → BIP Connection
Before writing a BIP, a Functional Behavior Assessment (FBA) must identify the function of the behavior — what the student is communicating or avoiding through their escalation. A BIP that doesn’t address function will not work. Most school behavior escalations function around escape from demand, sensory overload, or unmet social-emotional need. The de-escalation plan must address the function, not just the topography of the behavior.
Frequently Asked Questions
What is behavior de-escalation in the classroom?
Behavior de-escalation in the classroom refers to a structured, adult-led approach to reducing the intensity of a student’s emotional or behavioral crisis by modifying the environment, reducing demands, using regulated adult presence, and applying co-regulation techniques — rather than reactive discipline or consequence-based responses.
How is de-escalation different from discipline?
Discipline teaches rules and accountability. De-escalation restores regulation so the student can eventually learn. Discipline applied during a crisis activates the threat response and re-escalates behavior. De-escalation lowers physiological arousal first, which makes learning — and accountability — possible afterward.
How long does a classroom de-escalation take?
The active de-escalation phase (from agitation to beginning recovery) typically takes 10–25 minutes for most students. Peak behavior can last 2–10 minutes. Full recovery and readiness to re-engage academically may take 30–45 minutes. Timing varies by individual student, diagnostic profile, and severity of the trigger. Never rush the recovery phase.
What do I do if de-escalation isn’t working?
If a student does not begin to de-escalate after 15–20 minutes of the protocol, and no immediate safety concern exists, maintain safe distance, remove peers, and contact the school counselor, behavior specialist, or administrator. Do not attempt verbal escalation. Document the sequence of events for the behavior team to review and update the BIP accordingly.
Can de-escalation strategies work for nonverbal students?
Yes. De-escalation is primarily non-verbal. Regulated presence, environmental modification, demand reduction, and co-regulation tools (weighted blankets, fidgets, movement) do not require verbal communication. For AAC users or nonverbal autistic students, pre-agreed visual signals or AAC phrases can replace verbal empathy statements at Step 5.
Should de-escalation strategies be the same at home and at school?
Consistency across environments is the strongest predictor of regulation improvement. The IEP or BIP should be shared with parents so home strategies mirror school strategies. The specific tools may differ (a calm corner at school vs. a bedroom at home), but the principles — safety, demand reduction, empathy, debrief — should be identical.
5 Things You Can Do Tomorrow Morning
- Map your student’s escalation cycle. Take 10 minutes before school to write down one student’s specific warning signs for each phase. Early warning recognition is your most powerful tool.
- Practice one sentence. Choose your empathy statement for tomorrow: “Something got really big right now. No demands yet.” Practice saying it in a calm voice. The words matter less than the tone.
- Designate a regulation space. Clear a corner of your classroom and add one sensory tool. Label it “Calm Space” — not “Time Out.” Tell your class it’s there for anyone who needs it.
- Teach the signal system. Create a simple 3-color card system (green/yellow/red) or a quiet gesture students can use to signal overwhelm without speaking. Introduce it during morning meeting.
- Request or review the BIP. If a student is escalating regularly and has no Behavior Intervention Plan, send a written request to your team today. If a BIP exists, re-read it and check whether the de-escalation steps match what you’re actually doing.
Sources
- Walker, H. M., Colvin, G., & Ramsey, E. (1995). Antisocial Behavior in School: Strategies and Best Practices. Brooks/Cole. [Escalation cycle model]
- National Center on Positive Behavioral Interventions and Supports. (2023). Tiered Systems of Support for Behavior. PBIS.org. https://www.pbis.org
- Child Mind Institute. (2024). Helping Kids Who Struggle with Self-Regulation. childmind.org
- CHADD. (2024). ADHD and Classroom Behavior: Resources for Educators. chadd.org
- ADDitude Magazine. (2024). Emotional Dysregulation and ADHD in Adults. additudemag.com
- National Institutes of Health / PMC. (2023). Behavioral Intervention and Escalation Prevention in School Settings. ncbi.nlm.nih.gov
